Ductal Carcinoma in Situ (DCIS) is an early form of breast cancer. With DCIS, cancer cells are present in the breast duct, but they can’t spread to the surrounding breast tissue.
Ductal Carcinoma in Situ (DCIS) is an early form of breast cancer. With DCIS, cancer cells are present in the breast duct, but they can’t spread to the surrounding breast tissue.
At the moment, everyone diagnosed with DCIS receives treatment. However, we know that around half of all cases won't become invasive and may not cause harm.
Research is working to better understand this type of breast cancer. But what are scientists working on, and how could research help us treat it the future?
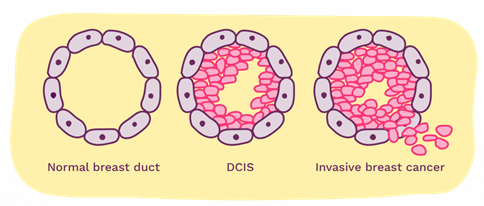
How can we understand DCIS better?
Currently, we can’t predict which DCIS cases will become invasive breast cancer. So, researchers are trying to understand how some cancer cells escape the breast duct and become invasive.
Scientists, using samples from our Tissue Bank, brought us one step closer to the answer last year. They found that the physical changes in breast cells play an important role in DCIS progressing to invasive breast cancer. They found some cells can act as a sheet around the DCIS tumour and separate the cancerous cells from the rest of the breast. These cells can prevent the tumours from growing larger and spreading.
And a group of international researchers, building upon previous work we funded, discovered that almost 1 in 5 breast cancers discovered after DCIS treatment aren’t genetically related to the original DCIS. This means these breast cancers aren’t recurrences, but new breast cancers.
Research like this can help scientists understand what triggers DCIS to spread beyond the breast duct, and cause harm.
Avoiding unnecessary treatment for low-risk DCIS
Researchers are also trying to better understand which DCIS cases aren’t harmful. This could help people skip treatment which may be unnecessary.
Dr Kastytis Sidlauskas is using artificial intelligence (AI) to more accurately predict which DCIS will go on to become invasive breast cancer. In the future, this approach could be used in clinics, to determine who needs immediate treatment and who could safely skip it and be monitored instead.
Appropriately treating high-risk DCIS
If we know that DCIS is likely to become invasive breast cancer, we need to make sure that treatment can stop it.
Currently, DCIS cases limited to a small area are usually treated with breast-conserving surgery, which removes only the affected area of the breast. Whole breast radiation therapy is then given to women who have a higher chance that their DCIS will return. This is given to make sure the DCIS doesn’t come back and progress to invasive breast cancer.
Researchers leading a large international trial want to find out if an extra boost of radiation could help prevent DCIS coming back. Recent results showed it reduced the chances of higher risk DCIS returning in the same breast. Now, Professor Ian Kunkler, from the University of Edinburgh, wants to follow up with UK participants of the trial to see if these benefits are maintained long-term.
The results of this trial will establish whether the extra boost dose of radiotherapy decreases the chance of DCIS either coming back, or progressing to invasive breast cancer. This will help doctors identify the best way to improve chances of survival for individual patients, whilst maintaining good quality of life.
There's still more to learn about DCIS. And research is helping us better understand this form of the disease, so we can develop new and better ways of treating and diagnosing it. We’re excited to see where DCIS research takes us in the future.