Learn about how breast cancer treatment may affect your chances of becoming pregnant and find out where to get support.
1. Will breast cancer treatment affect my fertility?
Fertility is the ability to get pregnant. Some breast cancer treatments, such as , can affect your fertility.
If having children of your own – or extending your current family – is important to you, you can opt to have fertility preservation before you start treatment.
It’s important to discuss this with your treatment team before any treatment starts.
It can be hard to decide whether to have fertility preservation and you may feel under pressure to decide quickly. It can be helpful to talk to someone about how you feel – see the “Further support” section at the end of this page.
Fertility in men
Men who are treated for breast cancer may also want to discuss fertility preservation options. See our information about breast cancer in men to learn more about this.
Chemotherapy
Treatment aimed at destroying cancer cells using anti-cancer drugs.
2. Referral to a fertility specialist
If having children, or more children, in the future is important to you, your treatment team should offer you a referral to a fertility specialist to discuss your fertility options. This should be as soon as possible after diagnosis to reduce delays in starting your treatment.
Taking time to think about questions you want to ask ahead of your appointment with the fertility specialist can be useful. If you have a partner, you may find it helpful to include them in the discussion. But it’s important to make the right decision for you.
Find out more about what happens at a fertility clinic.
Questions to ask your fertility specialist
- Can I check if I’m fertile before my breast cancer treatment starts?
- How will my age affect my fertility?
- What are my chances of getting pregnant after treatment?
- How long after treatment will I have to wait to find out if I’m still fertile?
- How can I try to preserve my fertility?
- Will I be able to have fertility preservation treatment on the NHS (including embryo or egg storage)? If not, how much will it cost?
- What does fertility preservation treatment involve?
- How successful are the different methods of preserving fertility?
- Can I use a sperm or egg donor?
- If I already have children, will I be eligible for fertility preservation treatment?
If you were not offered an appointment with a fertility specialist before your treatment started, ask your treatment team to refer you as soon as possible. This will help you get the support you need when your treatment finishes.
For a list of fertility clinics in the UK, see the Human Fertilisation and Embryology Authority (HFEA) website.
NICE guidelines
NICE (National Institute for Health and Care Excellence) is an independent organisation that provides evidence-based guidance on effective ways to prevent, diagnose and treat ill health.
NICE guidelines for assessing and treating people with fertility issues recommend that women with breast cancer:
- Have the chance to discuss the impact of cancer and its treatment on future fertility with their treatment team at the time of diagnosis
- Be offered appropriate procedures to preserve fertility if their breast cancer treatment may lead to loss of fertility, as long as they’re well enough to have the procedures, it will not worsen their condition and there’s enough time before cancer treatment begins
NICE guidance applies to England and their breast cancer guidance was last updated in 2023. If you’re in Wales, Scotland or Northern Ireland, talk to your treatment team or GP for more information as the guidance may differ.
3. Fertility in women
The information below may help you understand how breast cancer treatments might affect your fertility.
You are born with a set number of eggs in your ovaries (you do not produce new ones). This is known as your ovarian reserve.
By the time you reach puberty, the number of eggs you have will have decreased. It continues to decrease as you get older. The quality of your eggs also declines with age, affecting fertility.
Normally, 1 egg is released each month from the ovaries. Pregnancy occurs if the egg is fertilised by a man’s sperm and then implants itself in the womb. If the egg is not fertilised, you have a period.
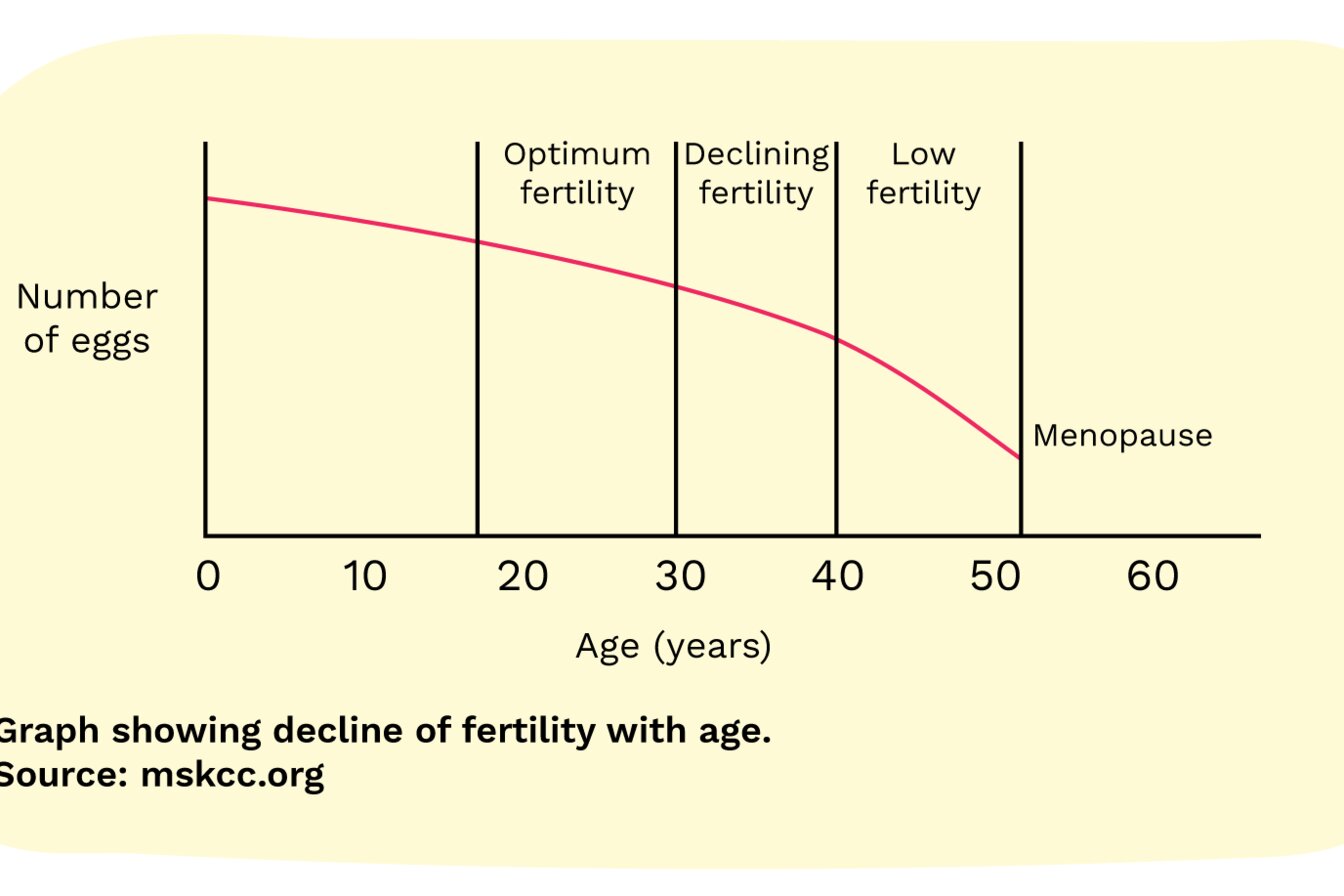
The ovaries stop releasing eggs and monthly periods stop when a woman reaches the menopause. The menopause is a natural event for all women and usually occurs between the ages of 45 and 55 years, with 51 being the average age in the UK. Studies show that women with an altered breast cancer gene (BRCA) may experience an earlier menopause.
The graph below shows how the average woman’s fertility declines with age until she reaches the menopause. How fast this happens will vary from person to person. It can also be affected by certain breast cancer treatments.

4. Chemotherapy and fertility
Can chemotherapy cause infertility?
Chemotherapy causes changes in your ovaries, reducing the number and quality of your eggs, which can affect your ability to become pregnant. It can also stop your periods. This may be temporary or permanent.
The likelihood of chemotherapy having lasting effects on your fertility in the future will depend on the drugs you’re given, the dose, your age and what your fertility was like before cancer treatment.
Which chemotherapy drugs affect fertility?
The chemotherapy drugs most likely to affect your ovaries are a group called alkylating agents. One of these (cyclophosphamide) is commonly used in combination with other chemotherapy drugs to treat breast cancer.
The effect of some other chemotherapy drugs, such as taxanes (docetaxel and paclitaxel), on fertility has not been as widely studied, but evidence suggests they may also affect fertility.
Will I stop having periods during chemotherapy?
Your periods might stop temporarily during your treatment and restart months or sometimes a year or more after your treatment has finished.
If your periods return after chemotherapy, it’s still likely you will go through an earlier menopause. In general, the younger you are when having treatment – particularly if you’re under 35 – the more likely it is that your periods will return.
If you’re over 35, your fertility may be reduced after chemotherapy due to a combination of your treatment, age and number of eggs.
If your periods return it doesn’t always mean you’ll be able to get pregnant. It’s important to speak to your treatment team if you have any concerns.
5. Hormone therapy and fertility
Can you become pregnant while taking hormone (endocrine) therapy?
Hormone therapies block or stop the effect of oestrogen on breast cancer cells.
Some of the most commonly used hormone therapy drugs for pre-menopausal women with breast cancer include:
- Tamoxifen
- Ovarian suppression such as goserelin (Zoladex)
- Aromatase inhibitors (anastrozole, letrozole and exemestane)
In most premenopausal women who take tamoxifen, the ovaries continue to work. When you start taking tamoxifen it may stimulate the release of the egg from the ovary (ovulation) and could make you more fertile. However, getting pregnant while on tamoxifen is not recommended.
Continued use of tamoxifen can make your periods less regular, lighter or stop altogether.
Ovarian suppression drugs such as goserelin switch off the production of oestrogen from the ovaries. They are given alongside hormone therapies such as aromatase inhibitors and tamoxifen.
Hormone therapy is usually taken for 5 to 10 years.
While you’re taking hormone therapy, you’ll be advised not to get pregnant as it may harm a developing baby.
Even if your periods stop while you’re taking hormone therapy you could still get pregnant.
Interrupting your hormone treatment to try to get pregnant
If you’re offered hormone therapy, it’s usually taken for 5 to 10 years, by which time you may be facing a natural menopause. Therefore, some women choose to take a break from hormone therapy if they want to try to get pregnant.
An ongoing study suggests a temporary break from taking hormone treatment to have a baby is safe for some women. Talk to your treatment team if you’re thinking about having a baby.
Many treatment teams advise women to wait for at least 2 years before becoming pregnant. This is because the possibility of the cancer coming back can lessen over time, and you may be at greatest risk in the first 2 years after diagnosis. If you’d like to take a break from your hormone therapy before 2 years, speak to your treatment team.
If you stop your treatment temporarily, you’ll still need to finish the remaining treatment in the future. For example, if you’ve been prescribed hormone therapy for 5 years but stop after 3 years to try for a baby, you’ll then need to take it for 2 years once you’ve restarted it.
Will I stop having periods during hormone therapy?
Hormone therapy may cause your periods to stop.
Your periods should start again once you stop taking hormone therapy as long as you have not gone through the menopause naturally while taking the drug.
It may take 3 to 6 months for your periods to become regular again, although this may take longer for some people.
Due to the length of time taking hormone therapy, the side effects may hide the signs of a natural menopause. You may realise you have started or been through the menopause when you’ve finished taking it. In this case your periods may not return after you stop your hormone therapy.
6. Other breast cancer treatments and fertility
Immunotherapy and targeted therapy
There are many different types of immunotherapy and targeted therapy drugs. Whether you’re offered these will depend on the type of breast cancer you have.
These treatments are usually given for between 6 months and 2 years depending on your circumstances.
It’s not fully understood whether they affect fertility.
You should avoid becoming pregnant while having any of these treatments as they may cause harm to a developing baby.
If you’re considering trying to become pregnant when you’ve finished any of these treatments, discuss this with your treatment team. This is because the length of time you should wait before trying for a baby varies with each treatment and can be at least 7 months after completing the treatment.
Removal of the ovaries (oophorectomy)
Some women have their ovaries removed as part of their cancer treatment or as risk-reducing surgery if they have an inherited altered gene, such as BRCA1 or BRCA2. Alterations in these genes can cause both breast and ovarian cancers, so removing the ovaries reduces this risk.
If you have this operation, you cannot get pregnant (unless eggs or embryos have been frozen before surgery), but you can consider egg or embryo donation in the future. See our information on surgery to remove the ovaries.
If you’re worried about having an inherited altered gene and fertility, talk to your treatment team.
7. Contraception
It’s important to avoid getting pregnant while having breast cancer treatment, as treatment can harm a developing baby.
You’ll usually be advised to use a barrier method of contraception, such as condoms.
It may also be possible to use a coil (IUD or intrauterine device). Speak to your treatment team as not all types are suitable for women with breast cancer.
The contraceptive pill is not advised after a diagnosis of any type of breast cancer. This applies to both the “combined” pill and to the progestogen-only “mini” pill. You can still use the morning-after pill in an emergency as it’s a single dose of hormones and unlikely to affect your breast cancer.
It’s important to use reliable contraception throughout your treatment. However, if you plan to get pregnant while you are taking hormone therapy, talk to your treatment team about your options.
8. Useful organisations
British Infertility Counselling Association
A charity providing counselling and support to people affected by infertility. You can also find a counsellor in your area.
The Daisy Network
Voluntary nationwide support group for women who experience a premature menopause. Allows members to share information about their personal experience of premature menopause.
Fertility Friends
An online community discussing infertility, adoption, parenting after infertility and moving on.
Fertility Network UK
Provides support and information, and promotes awareness of fertility issues.
Save My Fertility
An American patient information resource provided by the Oncofertility Consortium.
9. Further support
Whatever your feelings, you don’t have to cope alone. Involving your partner, family and friends can be helpful. Your treatment team and breast care nurse are also there to give you information and support.
You may also find it helpful to talk things through with someone who’s been in the same position as you.
- Our Someone Like Me service – see below – can put you in touch with someone who’s had a similar experience to you
- Chat to other people with breast cancer on our online forum
- Meet other women at one of our Younger Women Together support events – see below
You can also call our free helpline (below) to talk to one of our specialist nurses.
Quality assurance

Find support
-
Call our free helpline
0808 800 6000If you have any concerns about breast cancer, or just want to talk, our specialist nurses are here for you.
Lines open: Monday to Friday - 9am to 4pm; Saturday - 9am to 1pm
-
Explore ways to talk to our nurses
It can be difficult to talk to someone in person about breast cancer concerns. Explore other ways you can ask a question.
-
Someone Like Me
You never have to face breast cancer alone. Find somebody who understands what you're going through with Someone Like Me.
-
Events for younger women with primary breast cancer
Younger Women Together gives you the chance to meet other women aged 20-45 who understand what you’re going through.